New Medical Study just published in the journal Cell: Non-lethal Inhibition of Gut Microbial Trimethylamine Production for the Treatment of Atherosclerosis
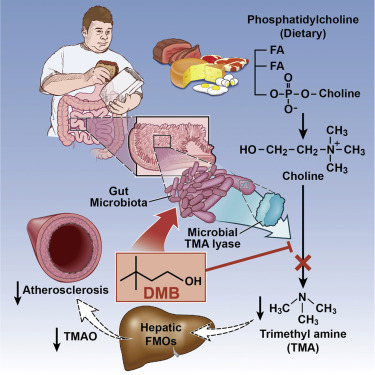 Image is courtesy of the journal Cell which retains the Copyright and any and all other rights. Used with permission for educational purpose.
Image is courtesy of the journal Cell which retains the Copyright and any and all other rights. Used with permission for educational purpose.
A new study just published in the peer reviewed journal Cell goes further into the research which we had posted about on Apil 08 2013. That 2013 post was titled : Intestinal microbiota metabolism producing Trimethylamine-N-Oxide (TMAO), may be a contributing factor in developing Cardiovascular Disease in Humans. That was an extremely important study which had been published in the peer reviewed journal Nature Medicine. Click on the previous line to read about that extremely important finding, as I believe that it presents a new foundation upon which we can potentially reverse Cardiovascular Disease in Humans.
The following are quotes about the new study from the journal Cell which was titled:
Non-lethal Inhibition of Gut Microbial Trimethylamine Production for the Treatment of Atherosclerosis
Highlights
•Gut microbial trimethylamine lyases are a therapeutic target for atherosclerosis
•3,3-dimethyl-1-butanol inhibits microbial trimethylamine formation
•3,3-dimethyl-1-butanol attenuates choline diet-enhanced atherosclerosis
•Non-lethal gut microbial enzyme inhibition can impact host cardiometabolic phenotypesSummary
Trimethylamine (TMA) N-oxide (TMAO), a gut-microbiota-dependent metabolite, both enhances atherosclerosis in animal models and is associated with cardiovascular risks in clinical studies. Here, we investigate the impact of targeted inhibition of the first step in TMAO generation, commensal microbial TMA production, on diet-induced atherosclerosis. A structural analog of choline, 3,3-dimethyl-1-butanol (DMB), is shown to non-lethally inhibit TMA formation from cultured microbes, to inhibit distinct microbial TMA lyases, and to both inhibit TMA production from physiologic polymicrobial cultures (e.g., intestinal contents, human feces) and reduce TMAO levels in mice fed a high-choline or L-carnitine diet. DMB inhibited choline diet-enhanced endogenous macrophage foam cell formation and atherosclerotic lesion development in apolipoprotein e−/− mice without alterations in circulating cholesterol levels. The present studies suggest that targeting gut microbial production of TMA specifically and non-lethal microbial inhibitors in general may serve as a potential therapeutic approach for the treatment of cardiometabolic diseases.”
The authors and researchers of this new Study were:
Zeneng Wang, Adam B. Roberts, Jennifer A. Buffa, Bruce S. Levison, Weifei Zhu, Elin Org, Xiaodong Gu, Ying Huang, Maryam Zamanian-Daryoush, Miranda K. Culley, Anthony J. DiDonato, Xiaoming Fu, Jennie E. Hazen, Daniel Krajcik, Joseph A. DiDonato, Aldons J. Lusis and Stanley L. Hazen
Click on this line to download the PDF of this new Study, from the Journal Cell’s website.
In laymen’s terms, this new Study (published in the journal Cell, showed that by lnhibiting the production of TMAO during the digestion process, clogging of arteries was vastly reduced in Mice. What worked in Mice could work in a similar manner in Humans. This study, in my opinion, adds a new layer to the very important knowledge foundation which was laid with the initial work published in the journal Nature Medicine (click here to view that post)
